We Must Ask Women About Birth Experiences
-
-
Rebecca Moore
Many women experience childbirth as traumatic. Yet childbirth related trauma and PTSD are often under-recognised and diagnosed. As Maternal Mental Health month draws to a close, Dr Rebecca Moore, perinatal psychiatrist and founder of Make Birth Better, explains how therapists can help
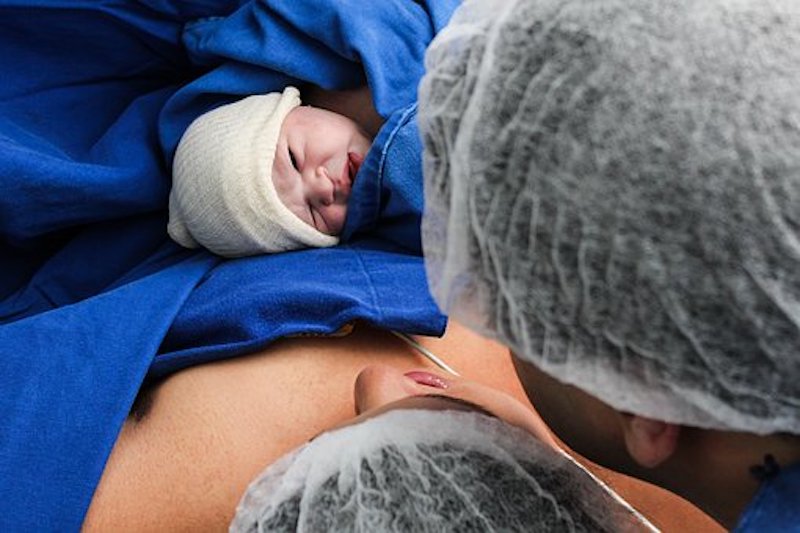
Women, Trauma & Mental Health Online Course
Learn women's trauma treatment methods from the world's leading experts
I was excited and felt blessed to be pregnant. I wanted to have my longed for IVF baby on a labour ward as I wanted an epidural and a full team around me in case something went wrong. When I went into labour, I ended up on the Home from Home Midwifery led unit. I didn’t know my midwife and she was really timid. The pain was unbearable and I had waves of panic and fear. My husband didn’t help me, and I felt so alone. After pushing for a long time they said I could go to the labour ward. I got out of the pool and ran there with no clothes on. I can’t believe I did this now, but I felt like I was fighting for my life.
I start this blog with one story. I have heard thousands over the past 20 years. They are powerful, shocking and upsetting, but these are the most important words in this piece.
Currently around 30 per cent of women find some aspect of their birth traumatic, which equates to around 200,000 women per year. We know that these women can go on to develop depression, anxiety or PTSD after a traumatic birth (Greenfield, M., Jomeen, J. and Glover, L. (2019) ‘It can’t be like last time’, Frontiers in Psychology.)
We need to do more to recognise the importance of new motherhood and to ensure that all families can access the right support when needed. This is the focus of our work at Make Birth Better, a national collaborative of professionals and parents all across the UK.
What should therapists know about birth trauma?
• When we talk about childbirth being traumatic, we mean that a woman, or anyone in the birth room, has found one or many aspect of their birth deeply upsetting and fearful.
• Symptoms of birth trauma can persist for weeks, months or many years.
• Around 1 in 25 women develop a clinical PTSD after birth.
• But birth trauma does not equal PTSD. Some women are traumatised by birth and do not develop PTSD, but they are still hugely affected on a day-to-day basis.
• Fathers, non-birthing parents and birth partners can also be traumatised by birth, as can anyone in the room at the time. We know that rates of trauma are high in midwifes and other maternity professionals, and that many are not being supported.
• Birth trauma and/or PTSD related to childbirth is often not well recognised or diagnosed. Many women are told that they have depression when they do not, or their experiences are dismissed – they are told that their baby is healthy, so they should get over it.
What contributes to birth trauma?
The cause of trauma is not necessarily what happens medically at birth, but how a woman is made to feel during birth. A study from 2018 found that, ‘what mattered to most women was
a positive experience giving birth to a healthy baby in a clinically and psychologically safe environment with practical and emotional support from birth companions, and competent, reassuring, kind clinical staff’ (Downe S, Finlayson K, Oladapo OT, Bonet M, Gülmezoglu AM, (2018) ‘What matters to women during childbirth: A systematic qualitative review’, PLOS ONE, 13(5)).
It is failings in how we are communicated with – such as a lack of compassion, or feeling unheard – that causes women to feel traumatised.
What is the impact of birth trauma?
When a person experiences birth trauma they will show many of the symptoms of PTSD: numbness, shock, feeling on edge and hypervigilant. They cannot understand what has happened and may feel like they are in a dream. Women are unable to stop thinking about the events of the birth, in their mind or in their sleep as nightmares. They may feel irritable and angry, or anxious and fearful. They may be terrified that something bad will happen to their family or baby, or they can feel completely disconnected from their baby.
Sometimes I meet women who have never spoken about their birth trauma, even though it happened twenty years ago. Symptoms may fade over time but often they do not, and a second pregnancy can cause things to reoccur.
What can therapists do to help?
Even if diagnosed, often women cannot access local, rapid, specialist treatment. The gold standard treatment for birth trauma is trauma focussed work, compassion therapy and/or EMDR.
But all therapists can help by helping women to talk freely about their birth, whatever their experience: good, bad or somewhere in between. Many women are never asked about their birth by anyone in detail. Doing this may unlock many issues that have been silenced for years. We need to give women time to tell their birth stories – and we need to listen hard.
Dr Rebecca Moore will be compering NIPS Presents: Mental Health, Children & Young Adults, a one-day seminar at Conway Hall, London WC1R on June 4. The event is aimed at both members of the public and mental health professionals. You can find out more about Dr Moore’s clinically-led education, campaigning and research work at Make Birth Better.